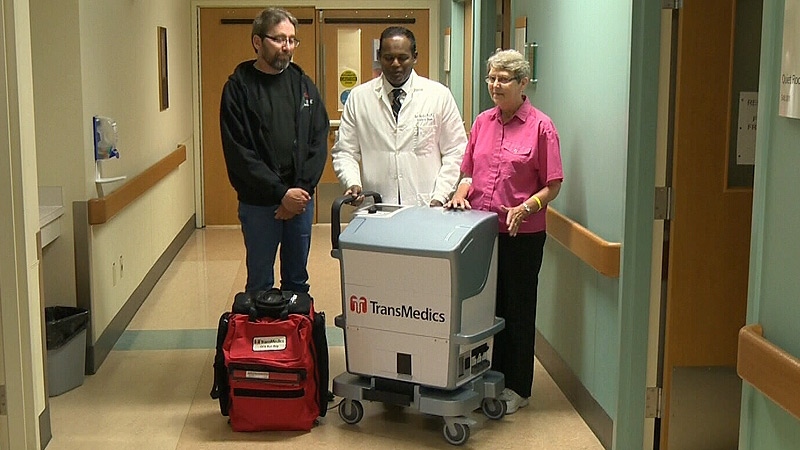
Canada’s only portable ex-vivo lung perfusion device is saving lives in Edmonton.
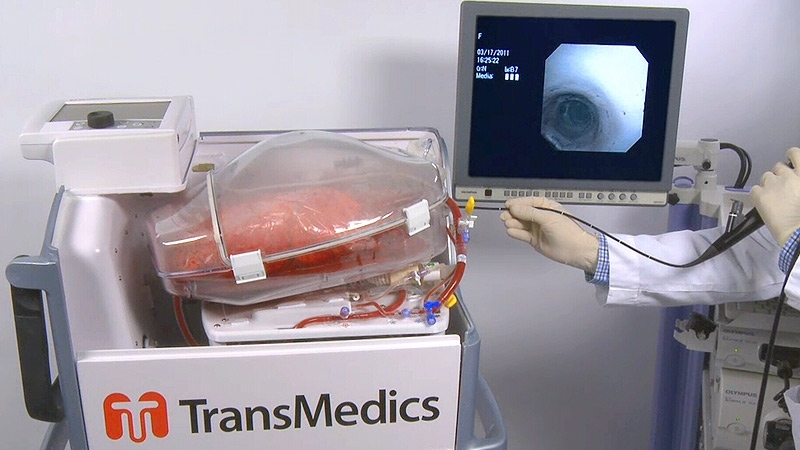
The device – home to the University of Alberta - mimics the processes of the human body and keeps donor lungs warm and oxygenated. Cardiothoracic surgeon Dr. Jayan Nagendran said the device provides an ideal environment to repair damaged lungs that could be used as transplants. Donor lungs are typically kept on ice.
“By having this portable, we were able to get rid of the ‘cold time’ and start repairing them the moment we took them out of the donor instead of waiting to get home to start repairing them.”
Dr. Nagendran said he took the device to the United States and successfully resuscitated a pair of donated lungs that no one in the country thought they could use.
“We are using only 1 in 4 lungs offered, so ... should we be successful in using more donors offered, we could rapidly decrease the death rate.”
About twenty-five Albertans die each year waiting for a lung transplant. Joyce Werk was close to being one of them.
“I was doing okay until about 2009, and then I started going downhill faster and I had to go on oxygen 24-hours a day.”
She was on a transplant waiting list for 3 ½ years before she finally got a call asking her whether she would take a damaged pair of lungs that had been repaired using the ex-vivo lung perfusion device.
“They were very poor at oxygenating, they had suffered from severe trauma so they were damaged,” said Dr. Nagendran. “Most of those things we were able to repair”
Fighting to survive, Werk accepted the lungs.
“It was a miracle for me,” Werk said. “Without it, I don’t think I would have made it.”
Dr. Nagendran said using the formerly damaged lungs was a difficult decision, but he felt confident after seeing the results of the repair.
“It was surreal because you have a life in the balance, and you have to make a very tough clinical decision to use something so novel and not done before.”
After having surgery in April, Werk can finally breathe again. She is looking forward to returning home to Beaverlodge, where she can see her grandchildren and start - what she is calling - her “new life”.
“Be able to go, and watch my grandkids play football again … and yell,” she said laughing.
With files from Carmen Leibel